Your cornea is one the most critical parts of your eye. It is the front-most transparent layer that provides about two-thirds of your eye’s optical power. It is also the eye’s most exposed and injury-prone part. Accordingly, it has the natural ability to heal most minor injuries. Sometimes, however, an injury, infection or other condition damages the cornea to the point where it cannot heal. This is when your ophthalmologist may recommend a cornea replacement surgery for you.
The cornea replacement surgery can correct many eye problems. Apart from injury and infection scars, it is also used to treat ulcers, keratoconus (a condition where your eyes bulge out), clouding, swelling or thinning of the cornea, as well as complications from inherited eye diseases and those caused by earlier treatments.
Preparing for your surgery
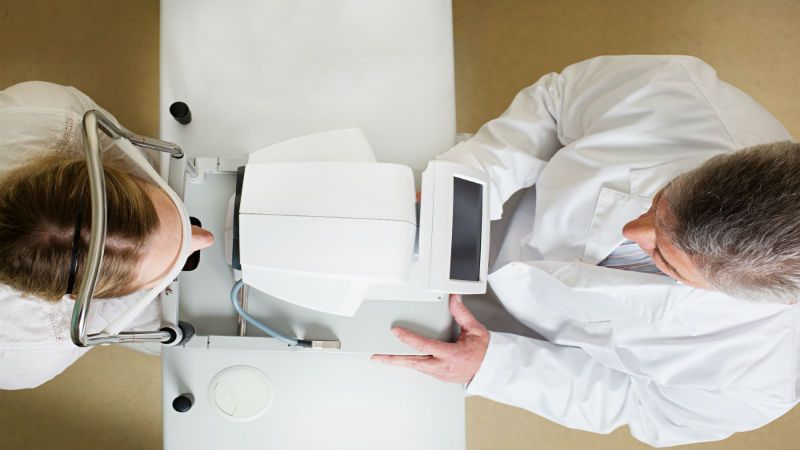
Once your doctor recommends that a corneal transplantation surgery is right for you, he/she will take steps to assess your condition and prepare you for the procedure. They will conduct a detailed eye exam and look for three key things.
- They will look for signs that can cause possible complications after the cornea replacement surgery.
- The second objective of this exam is to determine the measurements of your eye to see what size cornea is needed from a donor.
- Look for other eye problems that may need to be treated before or alongside the surgery. Your doctor will also review all your medications and may stop you from taking some for a few weeks before the procedure.
The surgical process
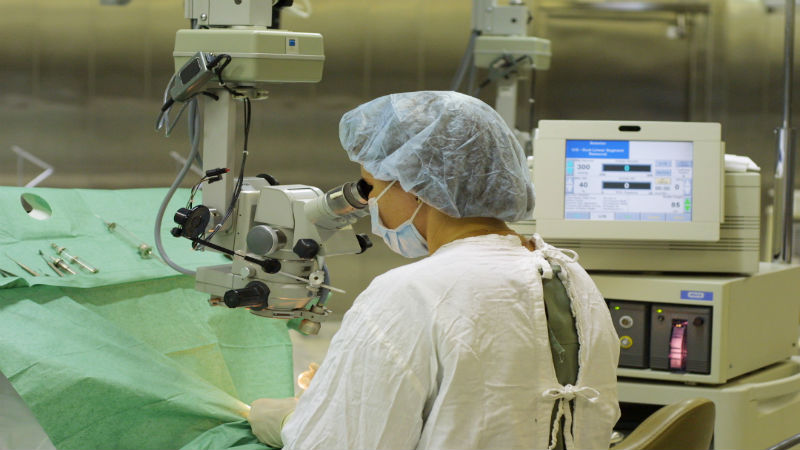
The corneal transplantation surgery is performed as an outpatient procedure, and the patient generally stays awake during the entire process. Here is a short glimpse of what happens once you are on the operating table:
- The surgeon inserts eye drops, medication and anesthesia to prevent pain and excess movement during the surgery.
- Then the surgeon will use a small device to keep your eyes open during the procedure.
- He/she will remove the damaged part of your cornea. The exact tissue removed depends on your case.
- The surgeon will then insert the donor’s tissue into your cornea and may insert stitches if necessary.
- Finally, the ophthalmologist will remove the device holding your eye open and will tape the eye shut to allow it to rest, heal and recover.
Recovery
You will be monitored after your procedure, the day after, and in the following weeks to ensure your treatment and recovery are successful.
After your surgery is complete, it is essential to follow your ophthalmologist’s instructions carefully. They may prescribe several medications to control complications, have you use an eye patch to protect the eye, and schedule several check-ups.
It is recommended you slowly work up to your normal routines and take special care to protect your eye from injury.
Complications and the importance of a good ophthalmologist
As with any surgery, there is a risk of complications. The greater the amount of donor tissue in your eye after the cornea replacement surgery, the higher the chances of your body rejecting the tissue. A good specialist will look for signs of rejection post-surgery and during follow-up and can catch symptoms early and treat it accordingly.
Other risks from the surgery include glaucoma, infections, bleeding, swelling of the eye and cataracts, among other things. Following up with the same professional who performed your procedure will ensure these complications are caught at an early stage and preventive measures are taken.